Harmful Chemical and Biological agents/substances
The agents/substances can be in different forms or transmitted in various ways such as dusts, gases or fumes that are breathed in, or liquids, gels or powders that come into contact with eyes, mucous membranes or skin and in some instances can be involuntarily ingested. Finally, some agents may be unintentionally injected or transmitted by animal stings, bites or excreta.
Harmful agents/substances can be present in anything from paints and cleaners as well as in water, flour or other dusts, solder fume, air conditioning systems, blood and waste.
Ill health caused by these agents/substances used/generated at work is preventable. Many agents/substances can harm health but, used properly, they almost never do.
Case study
| A hairdresser was diagnosed as suffering from irritant contact dermatitis caused by wet work. His hands were painfully itchy, and they would also scab over and bleed. What the employer has done? The employer has introduced a hand-care regime. This includes wearing suitable gloves when washing clients’ hair and using chemicals. Workers understand about good hand care, including washing chemicals from their skin promptly, drying their hands thoroughly and moisturising them throughout the day. The staff have regular skin checks to make sure any problems are spotted and treated early on. These measures have helped to control the dermatitis and allowed the hairdresser to continue working in the job he loves. |
What are the hazards?
Some agents/substances can cause asthma or other diseases, including cancer. Many can damage the skin, and some can cause serious long-term damage to the lungs or other organs.The effect can be immediate, such as dizziness or stinging eyes, or gradual over hours or several days in case of bio contamination for example, or can take many years to develop, such as lung disease. Many of the long-term or chronic effects cannot be cured once they develop.
What should employers do?
Employers should adequately control exposure to agents/substances, both chemical and biological, in the workplace that cause ill health. This means:- identifying which harmful agents/substances may be present, used or generated, in the workplace;
- deciding how workers might be exposed to them and be harmed;
- looking at what measures they have in place to prevent this harm and deciding whether they are doing enough;
- providing information, instruction and training;
- in appropriate cases, providing health surveillance.
This section explains how employers can carry out a risk assessment and how to decide on control measures.
How to carry out an assessment on agents/substances hazardous to health
This assessment concentrates on the hazards and risks from hazardous agents/substances in the workplace.Remember that health hazards are not limited to agents/substances labelled as ‘hazardous’. Some harmful agents/substances can be produced by the working process, e.g. wood dust from sanding, silica dust from tile cutting or clinical waste.
Identify the hazards
- Identify which agents/substances are harmful by reading the product labels and safety data sheets as well as taking into account the environment which may be inhabited by biological hazards e.g. pests/bacteria.
- If employers are in doubt they should contact their supplier.
- Include harmful agents/substances produced by the working processes, such as cutting or grinding, or to which workers may be otherwise exposed.
Decide who might be harmed and how
- How might workers be exposed? Think about the route into the body (whether the substance can be breathed in, get onto or through the skin or can even be swallowed) and the effects of exposure by each of these routes.
- Think of how often people work with the agent/substance and for how long.
- Think about anyone else who could be exposed.
- Don’t forget maintenance workers, cleaners, contractors and other visitors or members of the public who could be exposed.
- Also think about people who could be exposed accidentally, e.g. while cleaning, or what happens if controls fail.
Evaluate the risks and decide on precautions
Once employers have carried out an assessment and identified which harmful agents/substances are present, and how workers can be harmed, they need to think about preventing exposure. Following the hierarchy of risk control measures they should consider: - Do they really need to use a particular agent/substance, or is a safer alternative available?
- Can they change the process to eliminate its use or avoid producing it? If this is not possible, they must put in place adequate control measures to reduce exposure.
More information
If this is not possible the measures they adopt could include the following.
Changing the process (including the working environment) to reduce risks
- Considering whether they can change the process they use to reduce the risk of exposure.
- For example, could they reduce the temperature of a process to reduce the amount of vapour getting into the air or use pellets instead of powders as they are less dusty.
- Enclose the process or activity as much as possible to minimize the escape or release of the harmful agent/substance.
- Use closed transfer and handling systems, and minimize handling of materials.
- Extract emissions of the agent/substance near the source using extraction equipment e.g. local exhaust ventilation/fume cupboards.
- Restrict access to those people who need to be there.
- Plan the storage of materials, and use appropriate containers. Check that storage containers are appropriate and labelled and that incompatible materials, for example acids and caustics, are separated.
- Plan the storage and disposal of waste.
- Exposure to hazardous agents/substances can occur during cleaning, so plan and organize the workplace so that it can be easily and effectively cleaned.
- Smooth work surfaces will allow easy cleaning.
- Have the right equipment and procedures to clear up spillages quickly and safely.
- Clean regularly using a ‘dust-free’ method – vacuum, don’t sweep.
It makes sense for employers to record their assessment and to write down what steps they have taken to identify the risks. And the really important part is making a list of the actions they have taken to control the risks to workers’ health. This information should be supplied to workers who were not among those involved in carrying out the assessment.
The risk assessment should be regularly reviewed to ensure it is kept up to date to take into account any changes in the workplace.
Maintain controls
All elements of the control measures must be checked and reviewed regularly to make sure they continue to be effective. These checks should be adequate to determine whether improvements are required and will include:- maintaining plant and equipment – all ventilation equipment should be examined and tested regularly by a competent person (someone who has the necessary skills, knowledge and experience to carry out work safely). This may involve measuring the airflow or the pressures in the system, or air sampling in the workroom. In general, all extraction equipment must be examined and tested in accordance with national legislation;
- making sure systems of work are being followed and revising them if they are not working;
- making sure personal protective equipment is suitable (offering effective protection against the identified hazard), used, properly fitted and (where appropriate) maintained.
- making sure workers are properly vaccinated. Vaccination offers individual and collective protection.
Simple checks to control dust and mist
Fine dust and mist is invisible in normal lighting. It can be made visible with a ‘dust lamp’. Used correctly, a dust lamp is a cheap, powerful tool to help identify where dust problems such as leaks are and whether an extraction system is working effectively.The dust lamp should be set up to observe forward-scattering of light. Point the lamp to shine through the area where you think the dust cloud is. If possible, lower the background lighting by turning off workshop lights. Lock the lamp into the ‘on’ position and walk around the process, looking back up the beam at a slight angle, through the airborne dust:
- Note the settlement and spread of contamination on surfaces.
- Check the airflow indicator on the extraction system.
- Check for damage and leakage from the process.
- Speak to the operator and encourage reporting of any defects.
Case study
| A cook developed breathing problems after working with flour dust. She worked in a small, poorly ventilated room, with nothing to control her exposure to the flour dust. She became severely asthmatic and, after retiring early on health grounds, was awarded compensation. What the employer has done? The employer has since installed an extraction system to remove the flour dust and introduced new ways of working such as using a scoop to transfer flour, using sprinklers to spread flour and keeping the work area clean. The risk of other workers developing occupational asthma has been reduced. |
Ventilation
General ventilation
- All workplaces need an adequate supply of fresh air.
- This can be natural ventilation, from doors, windows etc. or controlled, where air is supplied and/or removed by a powered fan.
- If you work in an office or shop, natural ventilation will normally be enough to control dusts and vapours from cleaning materials etc.
- Air conditioning systems should be carefully maintained if not they can cause serious respiratory diseases (legionellosis).
- Sometimes planned, powered general ventilation is an integral part of a set of control measures, e.g. the welding of large fabrications in a workshop.
Local exhaust ventilation
- Local exhaust ventilation (LEV), or extraction, is an engineering control solution to reduce exposures to dust, mist, fume, vapour or gas in a workplace.
- A properly designed LEV system will draw dust, fume, gases or vapour through a hood or booth away from the worker.
- An extraction system should be easy for workers to use and enclose the process as much as possible.
- It should effectively capture and contain the harmful agent/substance before it is released into the workers breathing zone / working environment.
- Air should be filtered and discharged to a safe place.
- The system should be robust enough to withstand the process and work environment. It is important to maintain it and undertake tests to ensure it is working effectively.
More information
Things for employers to avoid when using LEV
Common errors in using extraction are:
- the effectiveness of small hoods is usually overestimated – be realistic;
- the hood is usually too far away from the process;
- the hood doesn’t surround the process enough;
- inadequate airflow;
- failure to check that the extraction continues to work;
- workers are not consulted, so they don’t understand the importance of extraction and do not use it properly.
Case study
| A worker in an electroplating factory developed occupational asthma. It was established that chemicals which can cause asthma were being used in the factory and contaminated air was reaching the workers. The worker had to take early retirement on medical grounds and was awarded compensation. What the employer has done? The employer has since installed an extraction system to remove the chemical fumes and the risk of other workers developing occupational asthma has been reduced. |
Simple steps to prevent skin damage
Employers can use the Avoid, Protect, Check approach:- void direct contact between unprotected hands and agents/substances, products and wet work where this is sensible and practical.
- Protect the skin. Avoiding contact will not always be possible so employers must remind workers to wash any contamination from their skin promptly. Businesses should provide soft cotton or disposable paper towels for drying the skin. Telling workers about the importance of thorough drying after washing. Workers should protect the skin by moisturising as often as possible and particularly at the end of the day – this replaces the natural oils that help keep the skin’s protective barrier working properly.
- Check hands regularly for the first signs of itchy, dry or red skin – when skin problems are spotted early they can be treated, which can stop them from getting too serious.
Case study
| Workers at a company using photographic chemicals developed a skin disease called ‘allergic contact dermatitis’. Symptoms of this condition include skin blistering, cracking, splitting, swelling and weeping. What should have happened? The employer should have considered using a different photographic chemical or designed and operated a process to avoid workers coming into contact with the harmful substance. The risk of other workers developing allergic contact dermatitis would have been removed or reduced. |
Workplace exposure limits
As well as controlling exposure to agents/substances hazardous to health, employers need to be aware that national legal limits may have been set on the amounts of many of the agents/substances that can be present in workplace air. These are known as workplace exposure limits (WELs) and relate to chemical substances.If the substance is known to cause cancer or asthma (check the label/safety data sheet), employers must control exposure to as far as is reasonably practicable.
Are employer’s controls adequate?
There are various ways of deciding this. A simple way to check is to use figure 2 below adapted from HSE’s guide to the Control of Agents/substances Hazardous to Health (COSHH) Regulations.For many harmful agents/substances, there is guidance available on good control practice from trade and industry associations and suppliers, as well as others.
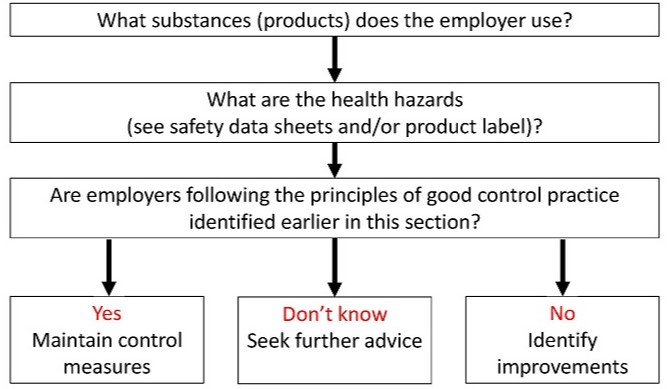
Figure 2 An assessment chart for checking whether controls are adequate
Personal protective equipment
Where employers cannot adequately control exposure by other means, they must provide personal protective clothing and equipment, in combination with other control measures.Employers must not automatically opt for personal protective equipment (PPE) as a control measure. It is not as reliable or effective as other measures.
Information and training
- Workers need to understand the outcome of the employers risk assessment and what this means for them. Employers must tell them what the hazards and risks are, and any workplace exposure limits, and what they need to do to protect themselves.
- Employers must inform workers of the results of any monitoring of exposure and the collective results of health surveillance.
- Employers should use the information contained in safety data sheets and other sources of information to train and inform workers.
- Workers should know what to do if there is an incident, accident (e.g. spillage) or emergency.
- Employers should involve your workers in developing control measures to make sure that they are suitable for the way they carry out the work as well as encouraging them to suggest improvements, and to report anything that they think might be going wrong.
- Employers should train workers in the correct use of controls and personal protective equipment.
- When a contractor comes into the workplace, they also need to know what the risks are and how the business is controlling them. In addition, the employer needs to know if they are bringing hazardous agents/substances onto the premises, and how they will prevent harm to their workers.
- It is helpful to keep basic training records.
Record and review
- Employers will find it useful to keep a record of what they have found out about the risks to health and the appropriate control measures.
- Write down where exposures occur, what the control measures are, and how they will maintain control.
- Keep an eye on things. Changes in equipment, materials or methods may require them to review their earlier decisions.
Find out more
- HSE’s Control of Substances Hazardous to Health (COSHH) website
- HSE's COSHH Essentials COSHH Essentials sets out basic advice on what to do to control exposure to hazardous substances in the workplace. It takes the form of straightforward advice in ‘factsheets’ called ‘control guidance sheets’.
- HSE’s simple step-by-step advice in HSE’s COSHH essentials
- Napo in... dust at work
- Napo in... danger: chemicals!
- Napo in... protect your skin!
- Napo in … lungs at work
Biological agents
Biological agents can cause diseases, infections, intoxications, allergies and even cancers.They are bacterial or viral microorganisms, prions, protozoa, yeasts, fungi and all their compounds. Biological risk also includes the transmission of disease between humans (HIV, Hepatitis, influenza...) or between animals and humans (malaria, dengue fever, weil’s disease etc.).
Biological hazards are present in most working situations, in particular health care, personal services, agriculture, agri-food industries, and outdoor activities which may be naturally contaminated, for example mosquitoes being present .
In most workplaces, the risk of catching a general infection, such as a cold or flu, is no higher than in any other public place and employers may not have to take any action. Nevertheless, to reduce the consequences of these diseases, particularly on vulnerable people, as well as induced absenteeism, for example vaccination campaigns against influenza is a good practice.
However, some people who work with animals, are exposed to pests working outside, who provide care for people, who work in laboratories, or who clean up or handle waste materials, may be exposed to harmful biological agents.
These can cause an infection if they are breathed in, swallowed, or if they penetrate the skin, and can include some very serious illnesses including cancers. Some may in turn cause an allergic reaction or are toxic (they produce a poison).
What should employers do?
Risk assessment is carried out by firstly identifying the hazard and then following the transmission chain from the "reservoir" (of the biological hazard) to the worker, secondly identifying risk control measures following the hierarchy of control; to reduce the exposure. The risk of exposure should be controlled as early as possible in the transmission chain.The risk assessment must consider how workers may be exposed to microorganisms (or to blood or bodily fluids, animals or animal products or waste materials which are known to carry micro-organisms). In general, unless it has been treated, employers should assume that human and animal waste materials, including sewage, may contain harmful micro-organisms that could cause an infection.
People who work outdoors should take precautions if they are working near stagnant water, which can carry harmful micro-organisms because of contamination. They may also be exposed to the risks generated from insects’ stings and animal bites.
Employers should find out about the common types of infection that are a risk for their relevant work activity (and how workers or others might be exposed), and decide whether they are doing enough to prevent this from happening.
The good news is that controlling the risk of infection is relatively straightforward – usually simple, good personal hygiene measures are often sufficient. All workers must have access to clean, adequate washing facilities.
Important control measures include:
- appropriate washable/disposable clothing;
- personal protective equipment (e.g. impervious gloves) and/or waterproof covering for cuts and abrasions;
- the right containers and safe systems of work for handling waste, including disposal of contaminated sharps (such as needles);
- work stations equipped with fume cupboards when working with contaminated materials:
- effective immunizations may be available. For example, hepatitis B vaccination is advisable if the risk arises from care work with people which might involve exposure to blood/bodily fluids.
Employers also need to provide information and training for workers and check safe systems of work are being followed, as above.
Case study
| A nurse took blood from a patient and then placed the soiled needle on the tray while labelling the blood samples. When the labelled samples were replaced on the tray the nurse contacted the used needle and suffered a needle stick injury. Fortunately, the needle was not contaminated with the harmful pathogens (for example HIV virus or the hepatitis virus etc.) What the employer has done? The employer has decided to introduce new procedures. Sharp boxes were added to the trays so that soiled needles could be placed in them immediately after injection or sampling. The employer also established a tri-therapy preventive care procedure in the event of needle stick injuries. |
Find out more
- Handbook on HIV and AIDS for labour inspectors
- Joint ILO/WHO guidelines on health services and HIV/AIDS 2005 contains 12 Fact sheets which provide a wealth of information useful to inspectors.
- HSE’s micro-organisms website
- Legionella and Legionnaires' disease This website provides practical advice and guidance to control the risks from exposure to Legionella in man made water systems
- Zoonoses
- Sharps injuries Sharps injuries are a well-known risk in the health and social care sector. Sharps contaminated with an infected patient's blood can transmit more than 20 diseases, including hepatitis B, C and human immunodeficiency virus (HIV).
- Waste managment and recycling: Occupational health issues